Bilharziasis
Bilharziasis (also called schistosomiasis) is one of the
most widespread human
diseases caused by parasites. This entry explains in general
terms what is
necessary for personal protection from bilharzia and for
ridding an area of the
disease. Further information from the references given is
needed. Cooperation
with government or other programs is essential.
An estimated 150 to 250 million people suffer from the
disease. It is found in
much of Africa, the Tigris and Euphrates valleys, parts of
Israel, northern Syria,
Arabia, Iran, Iraq, parts of Puerto Rico, Venezuela, Dutch
Guiana, Brazil, Lesser
Antilles, Dominica, Taiwan and parts of China, the
Philippines, Japan, and a few
villages in southern Thailand.
THE PARASITES
A basic understanding of the life cycle of the parasites,
called schistosomes, and
the characteristics of each phase is the first step in
preventing the disease (see
Figure 1).
fg1x186.gif (600x600)
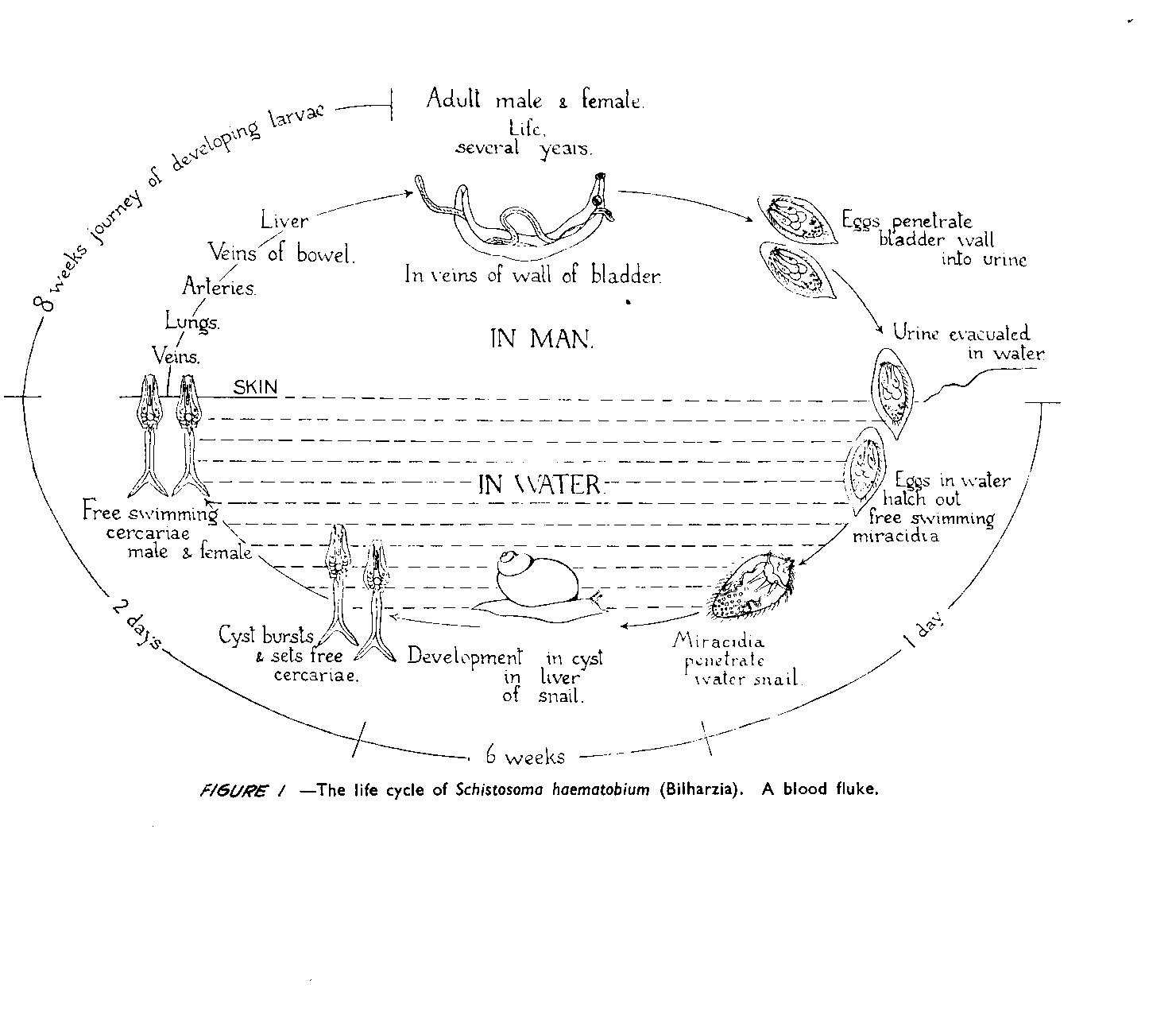
The disease has been found, besides in humans, in baboons, monkeys,
rodents,
water buffalo, horses, cattle, pigs, cats, and dogs. When
water is contaminated by
urine or feces from a victim of the disease, the eggs
contained in these hatch out
larvae that penetrate certain types of fresh-water snails.
In the snail host, the
larvae develop into cercariae, which work their way out of
the snail and become
free-swimming; this is the form that infects people. It can
survive in water for a
few days under favorable conditions.
The disease is contracted by contact with water containing
cercariae. Typical
ways are bathing, drinking, washing teeth, washing pots and
clothes, walking
through water, irrigating, and cultivating crops. Once the
parasite has contacted a
host, five minutes may be enough for it to penetrate the
skin.
It is important to note that bilharziasis cannot be passed
from human to human;
it depends on the snail intermediary. A victim must live in
or have visited an
area where the parasite is found.
SYMPTOMS AND DIAGNOSIS
At the spot where the parasite penetrates the host, a red
itching eruption lasting
several days usually develops. After the host is infected,
symptoms relate particularly
to the large bowel, the lower urinary tract, liver, spleen,
lungs, and the
central nervous system. The most characteristic symptoms are
bladder and colon
irritation, ulceration, and bleeding. Three to 12 weeks
after infection, a victim
will likely develop fever, malaise, abdominal pain, cough,
itchy skin, sweating,
chills, nausea, vomiting, and sometimes mental and neurological
symptoms. Later
developments may include frequent painful urination with
blood in the urine,
dysentery with blood and pus in the stool, loss of weight,
anemia, and enlargement
of the liver and spleen. Numerous complications are
possible.
Typically the acute phase subsides and host and parasite
live together over a
period of years, sometimes as long as 30, with the host
suffering a variety of
symptoms of intermittent and variable types. Bladder and
bowel troubles are the
most characteristic symptoms in this period.
The variety of vague and general symptoms is considerable
and may not be very
specific. Examination of urine and/or feces is very
important; special concentration
techniques may be necessary to reveal the eggs. Tissue tests
and skin tests
can be used by medically-trained personnel to identify the
disease.
TREATMENT
The disease can be treated with drugs, but only well-trained
persons should
undertake to treat a victim. Supportive treatment, which
includes good diet,
nursing care, rest, and treatment of other ailments and
infections, is important.
PREVENTION
The disease can be prevented by:
o Using
uncontaminated water-a properly built sealed well or an improved
sealed spring is
safe. (See section on "Water Resources.")
o
However, it is important to remember that all
water used must be safe.
Never bathe in or
touch water you wouldn't drink. Avoid suspected water. If
it is necessary
to use questionable water, boil it, or treat it with iodine or
chlorine. If you must
enter suspected waters, wear rubber gloves and wading
boots, and put
repellent on your skin; insect repellent (either diethyl
toluamide or
dimethyl phthalate), benzyl benzoate, cedar wood oil, or
tetmosol give
effective protection for about eight hours if applied to the
skin before
contact with the water. In case of accidental contact, rub your
skin immediately
with a dry cloth. Once cercariae have penetrated the skin,
no preventive
measures are possible.
o Chlorination-Chlorine
kills cercariae slowly, but properly chlorinated water
systems are
almost always free of the larvae. Use 2 halazone tablets in a
liter (quart) of
clear water; 4 tablets if the water is cloudy. In a water
system, use 1
part per million chlorine. Iodine is even more lethal to
cercariae. See
section on "Chlorination of Polluted Water."
o
Filtering-Cercariae are just big enough to be seen with the unaided eye,
and
can be filtered
from the water. However, dependence on filtration is
questionable,
since improperly made or operated filters will not only allow
cercariae to
pass, but may even provide a place for the host snail to live. In
short, filtering
is a poor technique.
o Storage-Storing
water at temperatures over 21C (70F) completely isolated
from snail hosts
for four days will allow the cercariae to die; at cooler
temperatures they
may live as long as six days. This is seldom a practical
approach.
Eliminating the snail intermediate host is at present the
most effective single
method of controlling bilharziasis. The following methods
are recommended:
o Use a sealed,
covered well or properly developed spring for a water supply.
Make sure it is
covered; this prevents access of organic matter that snails
eat, cuts out
light that would allow plants to grow for snail food, and
prevents infected
people from bathing in or contaminating the water.
o If surface water
must be used, put long-lasting (copper) screens on the
intake; draw lake
water far from vegetated shorelines, and preferably 2.4m
(8') deep; take
stream water from a fast moving spot.
o Be sure filters
and reservoir tanks are kept covered and dark and keep them
clean.
o Since snails
prefer the stagnant water of canals, irrigation ditches, and
dams, control has
been possible where the water level in ditches has been
varied, where it
has been turned off completely for periods, and where
canals have been
lined with cement or pipes have been used. Although the
latter is
initially expensive, it pays dividends not only in better health, but
also in less
water evaporation.
o Poison the snails
with copper sulfate, copper chromate, or other copper
salts. Use a dose
of 15-30 parts per million by weight of copper and try to
hold the
copper-treated water over the snails for 24 hours. All or most of
the aquatic
vegetation should be stripped from the stream bed or pool before
treatment.
Results for other than small controlled pools have been poor.
Before attempting
to treat streams, lakes, or other natural waters, study the
reference
material and seek experienced help.
RIDDING AN AREA OF BILHARZIASIS
Education is a major step in a continuing campaign against
bilharziasis. Basic
steps involved in improving your local waters so they will
not spread the disease
are as follows:
o Inform yourself.
Study this article, locate reference material cited below,
consult any
available health officials.
o Learn to identify
dangerous snails; for Africa, Professor Mozley's book is
very helpful. To
find the percentage of snails harboring schistosomes, collect
a large sample of
suspects (use rubber gloves, repellant, and snail scoop),
put individually
in test tubes or glass jars of water. Those shedding cercariae
are readily
detected, as the cercariae (0.5mm long and easily visible to
the naked eye)
are released in clouds. This test reveals only the snails
harboring mature
cercariae. Observe precautions at all times when collecting
and handling
snails!
o Find dangerous
snails locally, collect (again using rubber gloves, repellent,
and snail scoop)
and kill them. Mail empty shells to an expert to confirm
your
identification. Visit the expert if possible. Find out about government
or other programs
and participate in these.
o Make a personal
survey on foot (wearing boots) of local waters, using maps
and keeping exact
records to locate all dangerous snails. Local people can
often help here.
Aerial photographs are also helpful.
o Survey types and
intensity of bilharzia present in populace. Differences may
help localize
infection points. Keep special records for three- to six-year-olds,
who are the most
recently infected; these records will show most
accurately the
incidence of new infections.
o Educate the
public as much as possible, and get them to participate in the
program. Better
sanitation facilities, medical care, and improved nutrition are
critical, but improved
sanitary facilities are worthless if nobody uses them.
Encourage people
to live in villages away from infected waters, and to
construct
culverts or bridges at places where paths cross streams. The
number of such
crossings should be reduced. Any improvement should cater
to local customs
or offer an attractive alternative.
o Personally
supervise, participate in, and measure the effectiveness of
poisoning the
snails.
o Take continuing
steps to destroy the natural breeding places of snails,
particularly at
sites where humans and snails congregate. For example, the
place where a
stream crosses a road is a focal point: people stop to drink
and bathe; they
cook and wash out pots, providing food for snails. The
culvert and
embankments slow and impound the water, making ideal breeding
conditions.
Finally, a favorite sheltered place to defecate is under a bridge.
Filling in places
where water stands, changing drainage patterns, and
eliminating snail
food sources are possible techniques.
o Maintain a
continuing surveillance of focal spots and repeat poisoning
periodically when
necessary.
Sources:
Mozley, Alan. The Snail Hosts of Bilharzia in Africa: Their
Occurrence and
Destruction. London: H. K. Lewis & Co. Ltd.
Schistosomiasis, Bulletin No. 6. London: The Ross Institute,
The London School of
Hygiene and Tropical Medicine.
Acknowledgements:
Mason V. Hargett, M.D., Hamilton, Montana
Dr. Guy Esposito
Dr. Thomas W. M. Cameron, Montreal, Canada
Other References:
Craig, C. F. and Faust. Clinical Parasitology. Philadelphia:
Lea and Fibeger, 1964.
Hinman, E.H. World Eradication of Infectious Diseases.
Springfield Illinois:
Charles C. Thomas, 1966.
Markell, Edward K. and M. Voge. Medical Parasitology.
Philadelphia: W.B. Saunders
Co., 1965.
The Merck Manual of Diagnosis & Therapy. Rahway, New
Jersey: Merck.
Manson, Patrick. Tropical Diseases. Baltimore: William &
Wilkins Co., 1966.
In addition, up-to-date information can be obtained from the
World Health
Organization, Geneva, Switzerland.

